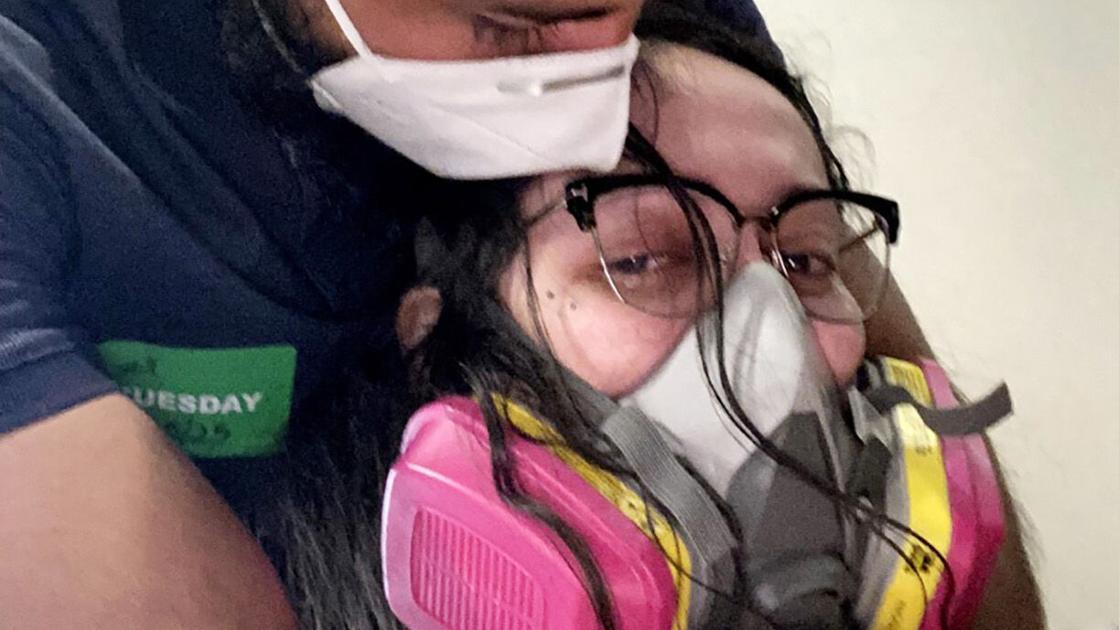
Selfie by Claudia Gutierrez, at the Mayo Clinic wearing a P100 to avoid chemical smells like hand sanitizer, with husband, Jesus.
Claudia Gutierrez had recently married, bought a new home and was excited about this next stage in her life.
Now she’s fighting daily to get back to the way she was before COVID-19.
Gutierrez, 28, started having symptoms in late December 2020, and tested positive Jan. 1. She was never really that sick: It was more like a bad cold, she says, and in no way as bad as the COVID long-haul symptoms she has now.
Terri Boitano, 62, was a swimmer and cyclist who most likely had asymptomatic COVID-19 in March 2020, not realizing anything was amiss with her health until early May that year.
And Tara Elliott, 46, did have a bad cough and fever when she got sick early in the pandemic, but she thought that was the extent of it — until three months later.
These Tucson women are examples of what University of Arizona health researchers found in a recent study on non-hospitalized COVID patients: The majority of individuals who experience mild or moderate COVID-19 infection also experience long COVID, or persistent sickness more than 30 days after they test positive.
”Wake-up call”
While other long-COVID research has typically focused on hospitalized patients with severe infections, this study published in early August looked at those who never had severe symptoms — or any symptoms at all.
Since May 2020, researchers followed over 6,000 Arizona residents who had COVID-19, as well as those who didn’t, through online surveys that recorded infection status, symptoms and any positive tests.
About 67% of those surveyed with mild or moderate infections go on to have “long COVID,” which means they are still having health challenges more than 30 days later, said Leslie Farland, an assistant professor with the UA’s Department of Epidemiology and Biostatistics.

Leslie Farland, assistant professor with the University of Arizona’s Department of Epidemiology and Biostatistics.
As time increased to 60 days, she said, the prevalence jumped to 77%.
Researchers found that, among other things, individuals with long COVID were more likely to have seasonal allergies and pre-existing health conditions than people without long COVID. The most common symptoms included chronic fatigue, shortness of breath, brain fog and an altered sense of smell. Those surveyed also reported insomnia, joint pain and muscle aches.
“This is a real wake-up call for anyone who has not been vaccinated,” wrote Melanie Bell, a biostatistics professor in the Mel and Enid Zuckerman College of Public Health, about the findings.
“If you get COVID, the chances that you’ll experience long-term symptoms are surprisingly high.”

Terri Boitano was a school psychologist and physically active before COVID. She had to retire her job and can no longer bike or swim.
”Tried to help”
Boitano said she most likely caught COVID very early on, when she traveled to California to care for her dying mother.
After returning, she was working at home as a school psychologist for the Flowing Wells School District and didn’t notice anything until nearly two months later, in May 2020, when she suddenly developed vertigo, headaches and sinus pain.
In hindsight, she’s not sure if she had COVID-19 then or if that was the start of her long-haul symptoms but she believes the latter. She was in the early stages of grief and so things were difficult to decipher.
What followed: her digestive system derailed, debilitating fatigue and burning skin on her arms that felt like a bad sunburn. Then she started to have pain in her feet that traveled up, into her shins, and it became hard to walk.
She eventually developed heart palpitations and was given a diagnosis of postural orthostatic tachycardia syndrome, commonly called POTS. In simple terms, POTS involves reduced blood volume when standing with symptoms including lightheadedness, fainting and rapid heartbeat.
Boitano estimates she’s seen about 20 doctors, most of whom were “super kind and tried to help.”
She kept hoping she could return to work but eventually she had to resign, ending a 13-year career with Flowing Wells. She is now considered officially disabled after long COVID became recognized as a disability under the Americans with Disabilities Act.
“I would say I have given up on seeing doctors,” she said. Instead, she said, she’s trying to accept that things will develop and then go away. “It seems,” she said, “that there’s really nothing that can be done.”
Boitano continues to have trouble concentrating and doing things as ordinary as reading and writing, watching television or listening to music with lyrics. She can’t swim laps or mountain bike anymore.
Emotionally? A month ago she was “very depressed,” she said, but right now she’s feeling more accepting.

Claudia and Jesus Gutierrez at home on Christmas Eve just days before she tested positive for COVID-19.
”A very complex post-viral syndrome”
The three Tucson women with long-haul COVID hope that as more people come forward with symptoms, it will be the catalyst for getting a speciality clinic started here.
For now, they said, it’s challenging to see multiple doctors at different locations who are scrambling to understand, based on their areas of expertise, how the virus harms the body over time.
“There’s a lot of cities that have built these large multidisciplinary clinics,” said Elliott. “That’s what we need, a well-educated team of doctors that understand the condition and can communicate with each other. This is a very complex post-viral syndrome that can affect all different parts of the body.”
Like the other two women, Elliott has had many different challenges. After being sick early on in the pandemic, she began to have shortness of breath again in June 2020. She now uses an inhaler — something she’s never used before in her life.
She used to play poker several times a week, enjoyed bowling and going to the movies but it’s too tiring right now to resume any of those activities. She’s also having vocal cord dysfunction, she said, and her voice sometimes gives out on her.
But one of the hardest things has been a lack a mobility: She’s been using a walker since July of last year due to leg pain.
“It’s like a charley horse in my legs and it just doesn’t stop,” she said. She started physical therapy recently and is hoping that will help.
“Our biggest fear, I think, is getting reinfected,” she said, explaining it’s “terrifying to think the long haul could get worse.”
“There’s still so much we don’t know,” she said.
The fear and uncertainty that accompany long haul is why Boitano would like to see not just medical services at one clinic, but also mental health services, to deal with the anxiety and depression that often accompany a health crisis.
Spokeswoman Rebecca Ruiz Hudman said Banner Health is working on plans to provide a long-haul clinic here.
“As more is learned about the residual effects of COVID-19, Banner is committed to ensuring communities have access to care at all points in their COVID journey,” said Ruiz Hudman, “and has plans to formally open a long-COVID treatment program that will be available to patients in Phoenix and Tucson in the near future.”
”Psychologically so difficult”
For now, Gutierrez travels to Phoenix regularly to see doctors at the Mayo Clinic there as well as Dr. Thea Davis, who works for Arizona Arthritis and Rheumatology Associates in Gilbert.
“We have been seeing more and more COVID long-haulers,” said Davis, whose clinic about two years ago started helping patients with one of Gutierrez’s diagnoses: Mast Cell Activation Syndrome, which cases the body’s mast cells to release an inappropriate amount of chemicals into the body, causing allergy symptoms and a wide range of other challenges.
It’s a common diagnosis for long haulers, she said.
“To be previously very very healthy and then to be suddenly debilitated is psychologically so difficult,” Davis said of Gutierrez, whose long COVID is the worst Davis has seen.

Claudia Gutierrez at Tucson Medical Center infusion center get her PICC line cleaned before she stopped tolerating fluids.
Often, Davis said, there’s already some sort of underlying chemical sensitivity the person might not have been aware of yet. Then, with the “viral insult” of COVID-19, the syndrome gets activated.
Like Boitano, Gutierrez has also been diagnosed with POTS but so far it’s not going away.
“I think there’s a lot of misinformation and fear surrounding long haulers,” Davis said. “The virus itself is not harmless but is everyone going to have really severe symptoms? No.”
But for people like Gutierrez, she said, the aftermath of COVID-19 is “very real and very debilitating.”
What Davis wants people to avoid is discounting other people’s experiences because theirs wasn’t the same.
“It’s very psychologically damaging,” she said, “to not be believed about the severity of it.”
Trevor Jones is family nurse practitioner at Immediate Care Arizona in Tucson, which is one of the first places Gutierrez went to in late January because she wasn’t feeling well and wanted help with her symptoms.
They provided infusion therapy to help her restore micronutrients that had been lost because her appetite was so suppressed.
“It would help for a while and then she’d come back and get another one,” he said.
They have seen about 10 long-hauler cases, he said, and Gutierrez is one of the worst.
“She had a lot of problems with medication. She was so sensitive to it that there weren’t really a lot of things that could be done to help her without having a reaction,” he said. “Eventually, she couldn’t even tolerate IV fluids.”
Gutierrez said she can now smell laundry detergent from 15 feet away, and cannot tolerate many of the pharmaceuticals that would help her.
She said she’s reaching out because she wants people to know the risks that come with contracting COVID-19.
“It’s been horrible,” she said. “I have one of the more severe long-haul COVID cases in the state of Arizona. I would not wish this on my worst enemy.”
Contact reporter Patty Machelor at 806-7754 or pmachelor@tucson.com